
18 Feb Eczema – An itchy situation
Food allergy cases are rising worldwide at an alarming rate, particularly in children. Although its occurrence could certainly be overestimated since the public often confuses an allergy disorder with other adverse food reactions, like food intolerance or food poisoning. Even so, allergic diseases are among the fastest growing chronic conditions in Australia.
According to the ASCIA (Australian Society of Clinical Immunology and Allergy), allergies affect 1 – 2% of adults and 4 – 8% of children under five years of age. More recent Australian data shows up to 10% of children will develop a food allergy in the first 12 months of life. That’s one of the highest rates worldwide! But there is some good news in this dire warning, as up to 85% of them overcome their allergy before they reach 5 or 10 years of age.
Still, having this alarming increase in allergy rates, both, parents and healthcare providers are asking themselves – Why are our children more likely to develop this adverse food reaction? Experts explain that current lifestyle and environmental factors may play a role, but what does that mean?
These days children may have less exposure to infections in early childhood (i.e. due to excessive hygiene, use of hand sanitizers, less outdoor play etc.) and this is associated with an increased risk of allergy. Other factors may include delaying feeding infants certain foods that are potentially allergenic, impaired vitamin D status which can affect their immune system, the overuse of antibiotics or even giving birth by caesarean section, and many others that are under current scientific research.
Does this mean that my child is going to suffer from an allergy? What if I as a parent, suffer from allergies too?
Don’t panic! Let’s see what the evidence says.
In many cases, food allergies in children can follow cases of eczema or otherwise called, atopic dermatitis – an inflammatory skin disorder often linked with allergies. This condition is most common in children under 2 years of age (10-30%) and usually improves as they grow.
WHAT IS THE LINK BETWEEN ECZEMA AND ALLERGIES?
Eczema is characterised by a dry, itchy, red rash, that appears mainly on the arms, legs, hands, and face of your baby, but may also be found on other parts of the body. If one or both parents suffer from allergies or asthma, their children will be at a higher risk of developing eczema, suggesting that there are genetic factors implicated in the development of this ailment. Although there are many effective treatments, no cures are currently available.
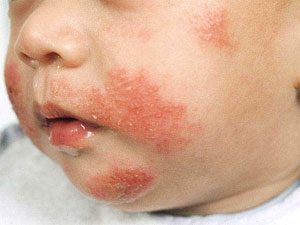
* Photo credit: http://www.babydermatitis.com/trigger-factors-baby-atopic-dermatitis/
It’s important for you to understand that this condition is not caused by any type of allergy but is associated with the development of future food and environmental allergies, or what allergists call the “atopic march“. This involves the diagnosis of atopic dermatitis during your child’s first years of life, followed by food allergy (about 1/3 of cases), allergic rhinitis and asthma, usually in that same order. There is also very little role for food chemicals such as salicylates and amines causing eczema in infants.
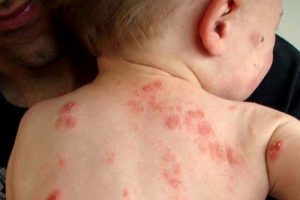
Photo credit: http://www.abc.net.au/news/2011-09-07/dad-holds-baby-with-eczema/2874486
So, what that means is if your child is diagnosed with eczema, he or she may
be more at risk for developing allergies or asthma as they grow. This not only includes environmental allergies (like pollen, mold, pets, dust mites), but also food allergies. The foods most often responsible for worsening atopic dermaticis are eggs milk, wheat and soy. Removal of the foods will not result in eczema cure, but it will prevent an immediate allergic reaction in your child. Diagnosis of food allergy in eczema is based on clinical history, IgE mediated testing followed by an exclusion diet and oral food challenge that should be supervised by an Accredited Practicing Dietitian and Allergist who oversees the testing.
OTHER THINGS YOU CAN DO FOR YOUR CHILD
Some children with atopic diseases benefit from food allergy tests and staying away from trigger foods that cause the outbursts. Remember that eczema doesn’t have a cure, but it can be successfully treated when supervised by an Allergist, so it’s important that you seek help from a proper specialist.
In some children with a severe condition, elimination diet or avoiding foods that trigger the symptoms may result in better eczema control, in this case, foods are re-introduced one at a time to determine if it causes the eczema to flare. If there is no improvement within two weeks on this regimen, it means that those foods are unlikely to be a problem. Important to note, that any elimination diet should be supervised by a Dietitian, as some infants are put on very restrictive elimination diets without improvement, which can cause poor growth and malnutrition.
Many infants with eczema experience growth failure, due to:
• Increased energy and nutrient requirements due to scratching, lack of sleep and skin losses
• Being on a restricted diet – often milk, egg and nuts are excluded
• Poor feeding – often breastfeeding is the only way to comfort these infants which leads to reduced intake of solid foods if they are at an age where solid introduction has occurred
• Inflammation due to allergy
A Dietitian will help you to adjust your child’s feeding or meal plan, telling you the number of calories and nutrients your baby needs and look for nutritious replacements to the foods they can’t eat. If you’re breastfeeding and your doctor doesn’t say otherwise, keep nursing your baby, as it will not only help to give important nutrients and immune factors to your baby, but it will also comfort them.
Remember to seek advice from a dietitian who is a specialist on allergies, given that an incorrect diet or putting your son on very restrictive elimination diet without need or improvement, will have adverse effects on his nutritional status.
TAKING CARE OF THE SKIN IS IMPORTANT!
There are other factors that can make the skin more susceptible to allergens and irritants, causing more damage and aggravating eczema symptoms. The most common of them are:
- Dry skin
- Scratching which can often lead to bacterial infections (night gloves and clipped fingernails may be needed in young children)
- Viral or bacterial infections
- Swimming in chlorinated swimming pools
- Playing in sand and particularly sandpits
- Sitting directly on carpets or grass
- Inhalant allergens
- Food intolerances to artificial color and preservative in some people
- Irritants such as perfumes, soap, chemicals, or synthetic fabrics
- Temperature changes (such as heat) or overly heated rooms or baths/showers
- Stress (this can make it worse, but eczema is not a psychological condition).
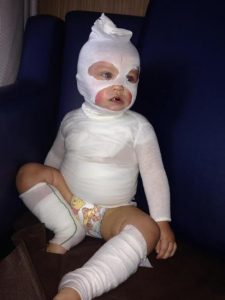
* Photo credit: http://www.bamboobubby.com.au/blog/wet-wrapping-to-help-eczema-in-7-easy-steps/
To help treat those skin conditions, your doctors may also prescribe some medication, including ointments, moisturizers, diluted bleach baths, topical steroids or antihistamine to soothe your child’s itchy or painful outbreaks, combined with wet dressings to wrap the exposed skin. Breastfeeding will also give comfort to your child and help to keep their immune system strong to minimise the reaction.
Finally, there are other types of inflammatory skin conditions similar to eczema. Some common examples you may have heard of before are angioedema, urticaria or contact dermatitis. But don’t get paranoid, it’s important to point out that these changes in the skin can be caused by other things besides an allergic reaction or adverse food disorder. One such example is the case of contact dermatitis, which it is caused by direct contact with irritants or chemicals like detergents, perfumes or cosmetics.
The bottom line is that some children develop allergies or have tendencies to develop conditions such as eczema that can lead into allergies, and they can be caused by many different reasons. If you believe your child is affected, be sure to talk to your Paediatrician.
REFERENCES:
- Food allergy: immune mechanisms, diagnosis and immunotherapy. Yu W, Freeland DMH, Nadeau KC. Nat Rev Immunol. 2016 Dec;16(12):751-765. https://www.ncbi.nlm.nih.gov/pubmed/27795547
- Epidemiology of food allergy. Sicherer SH. J Allergy Clin Immunol. 2011 Mar;127(3):594-602 https://www.ncbi.nlm.nih.gov/pubmed/21236480
- Australian Society of Clinical Immunology and Allergy. Allergy and the skin. https://www.allergy.org.au/patients/skin-allergy
- Food Allergies Part 1 lecture notes. National Paediatric Dietetic Training. Dietitians Association of Australia (DAA) & Child Health in Life and Disease Dietetics (ChildD). 2017 March.



Sorry, the comment form is closed at this time.